What if we considered mental health primarily in terms of strengths, needs and adverse events and considered diagnosis as a secondary indicator? I have been a consultant for Medicaid mental health systems for almost a decade, and one thing I can see from this experience is that primary diagnosis is fluid. It could be that misdiagnosis is prevalent. A 2012 study suggests that individuals with bipolar disorder could receive services for over a decade before being properly diagnosed (Hughes, 2016). It could be that many individuals do not meet the full criteria of one disorder or another. It could be that mental illness is still poorly understood, even with the introduction of the Diagnostic and Statistical Manual (DSM) V and ICD-10 coding.
I was in a room the other day talking about mental health care, and a member of the audience suggested that if we could just achieve accurate diagnosis by blood draw, the problem would be solved. Would it? If everyone had an accurate diagnosis of mental health disorder after the first visit to care, would that revolutionize mental health care? If we could put everyone in the appropriate diagnostic box, would we see better outcomes? It is likely that the benefit would be limited.
The Adverse Childhood Experiences Study (ACES, Felitti, 1998) highlighted the importance of traumatic experience and social support for wellbeing. Prior, George Engel (1977) illustrated the importance of considering biological, social and psychological aspects of mental disorder in what he termed the Biopsychosocial Model (BPSM). Today, we are still challenged to understand the underpinnings of mental disorder, its causes and its treatment.
What if we thought of mental health primarily in terms of strengths, needs, underlying trauma and past behaviors? Needs are problem areas for an individual which can be targeted for change. Strengths identify an individual’s personal skills to celebrate or to build. Underlying trauma represent exposures to adverse events, and past behaviors are prior actions by the individual which had a lasting impact.
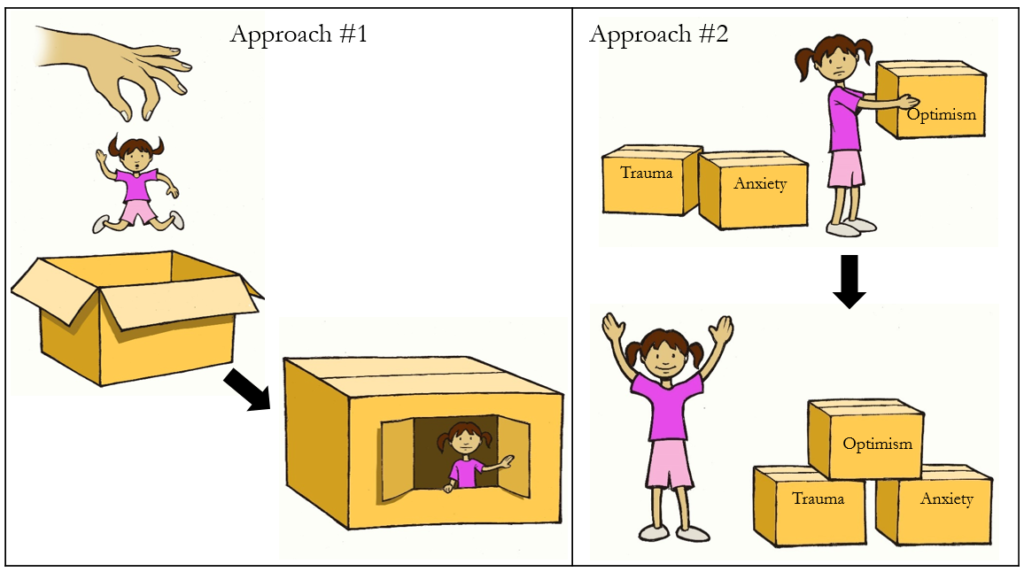
In this sense, optimism would be a strength to celebrate or build, anxious feelings a need to address, emotional abuse an adverse event to consider and suicide attempts, long prior, would be past actions to acknowledge.
Biological, social and psychological indicators could all be considered in terms of strengths, needs, underlying trauma and past behaviors. Familial predispositions to mental disorder can be a need, strong network of social support through friendships a strength, family dysfunction a need, victim of community violence (e.g., mugging) as underlying trauma, prior arrest as past behavior, and so on. As we begin to break down our stories into these building blocks, we can begin to unpack our boxes and rebuild our lives.
Let’s think outside the box.







